Latest news
Xiapex
St Peters Andrology is the first centre in the UK to offer Collagenase (Xiapex) treatment for Peyronies disease. Get in contact with us to arrange an appointment.
Read on...
Our new website
Welcome to our new website!
We hope you find it informative and useful. Let us know what you think!
Read on...


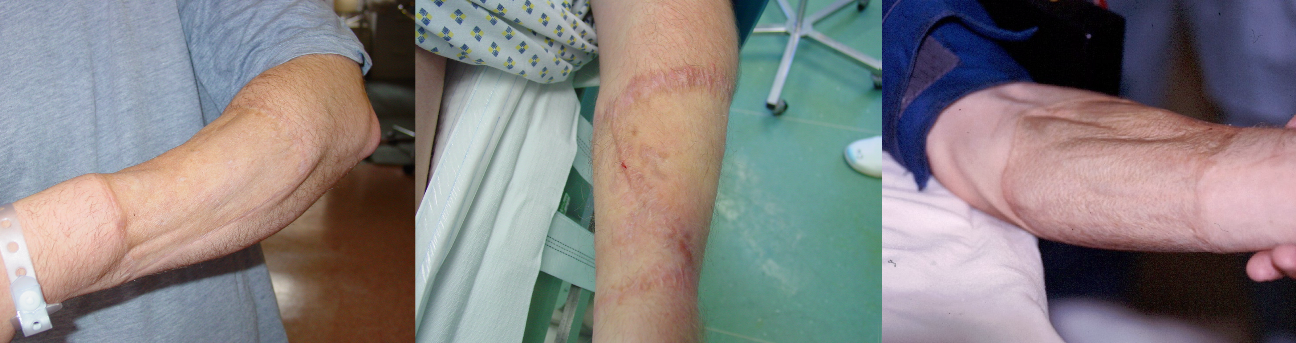
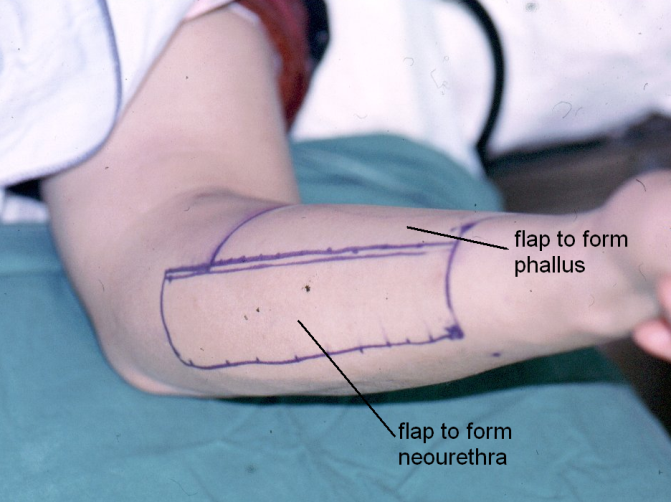
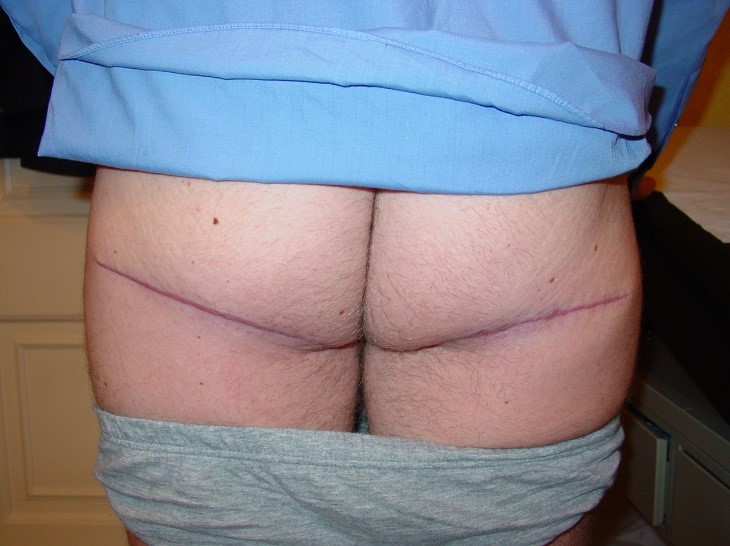
 We use lower buttock skin crease full thickness grafts for the forearm grafts instead of using groin skin, axillary skin or abdominal skin. The scar from buttock skin is easily hidden and the hair quality is fairly fine and appropriate for most forearms.
We use lower buttock skin crease full thickness grafts for the forearm grafts instead of using groin skin, axillary skin or abdominal skin. The scar from buttock skin is easily hidden and the hair quality is fairly fine and appropriate for most forearms.